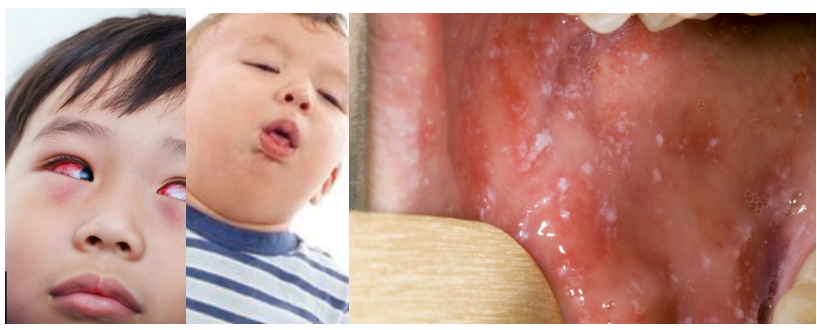
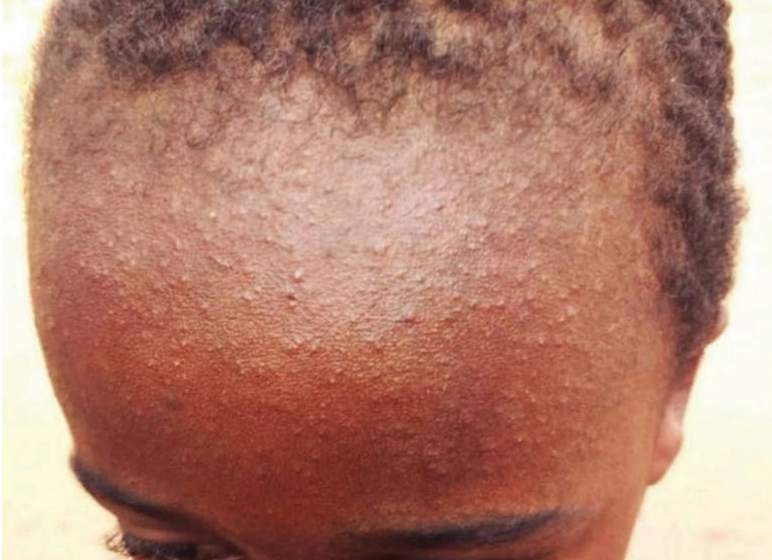
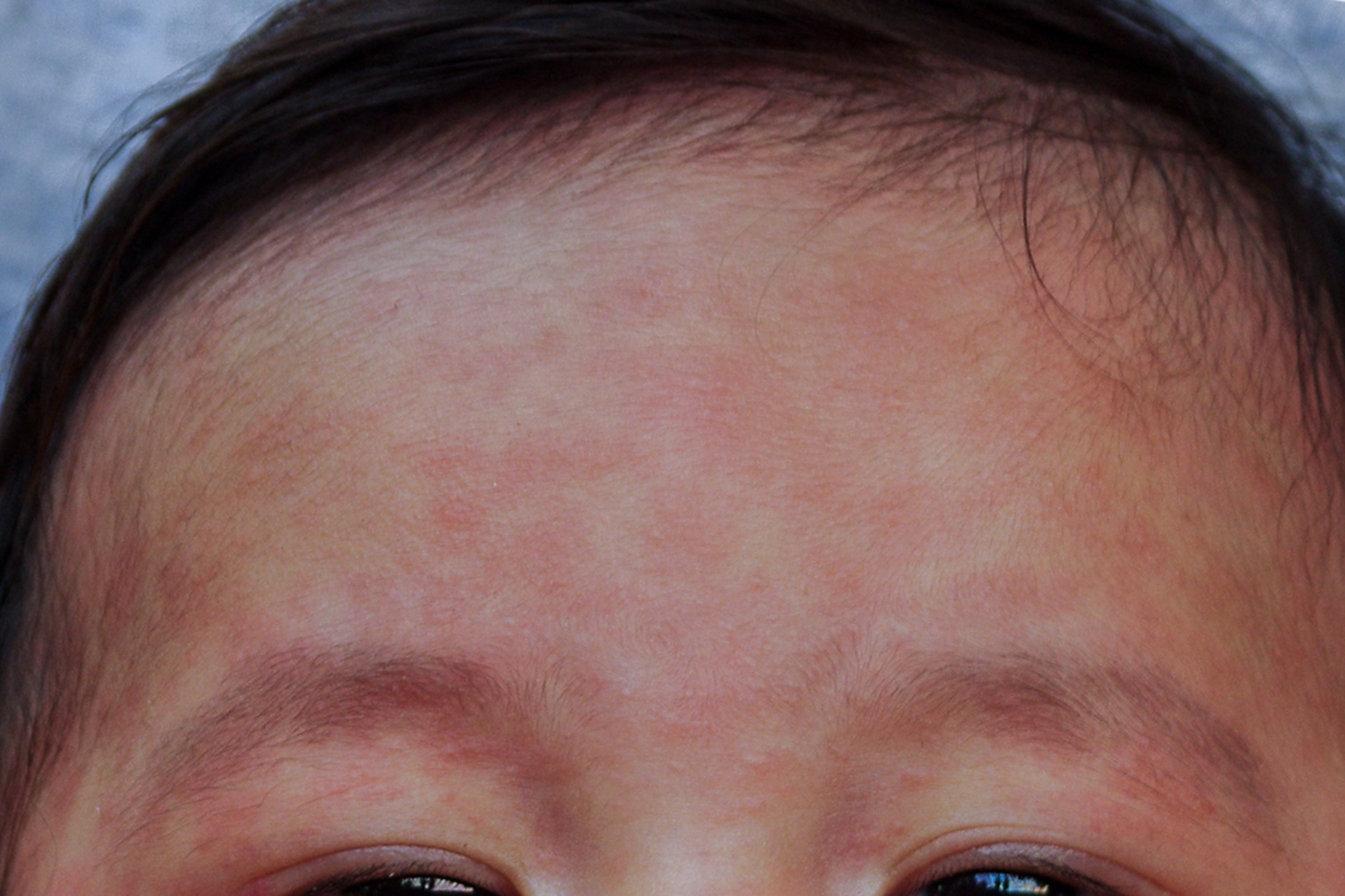
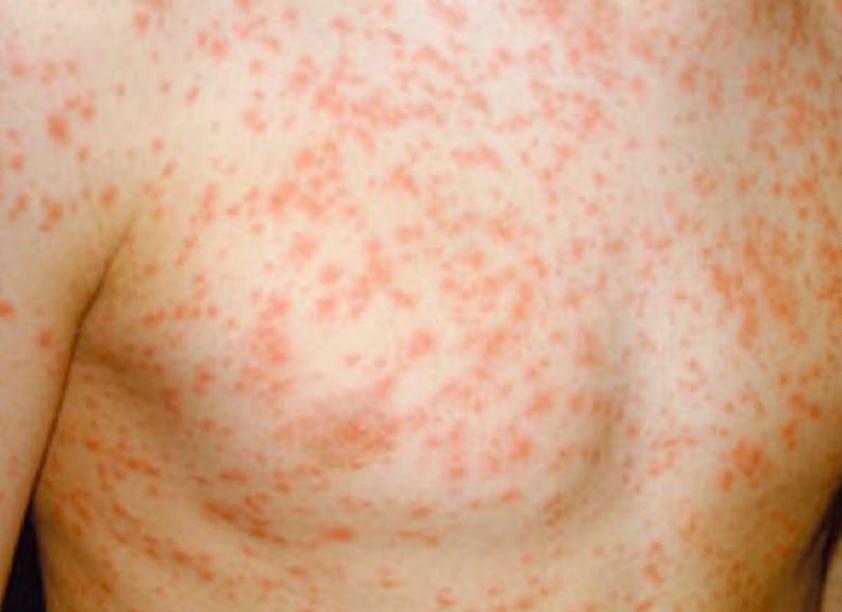
Even in developed countries such as the UK, around one in every 15 children with measles will develop more serious complications. These can include:
- ear infection (otitis media) in about 1 in 12 children with measles
- pneumonia (chest infection) in about 1 in 16 children with measles
- diarrhoea in about 1 in 12 children with measles
- encephalitis (inflammation of the brain): 1 case for every 1000-2000 children with measles. Encephalitis can lead to permanent brain damage
- measles causes death in about 1 in 5000 children with measles
In rare cases, measles can lead to a condition called SSPE (subacute sclerosing panencephalitis). This causes progressive destruction of the brain resulting in dementia, loss of motor function, fits (epilepsy), and eventually death. There is unfortunately no cure for SSPE.